Freedom from glasses starts here.
Keratoconus is a condition where the cornea progressively thins and bulges forward into a cone like shape. As the cornea becomes more irregular, vision can look blurry, stretched, or shadowed, and standard glasses may not fully sharpen it. Early diagnosis matters because treatments like corneal cross linking can slow or stop progression in many patients, helping protect long term vision.
Keratoconus affects the structure and strength of the cornea, which is the clear front window of the eye. When the cornea loses its regular shape, it cannot focus light cleanly onto the retina, which is what creates distortion.
With keratoconus, the cornea thins and becomes uneven, leading to irregular astigmatism. Instead of light focusing neatly at one point, it spreads across multiple points, which can cause blur, ghosting, and a sense that your vision is never quite crisp even with a current prescription.
Regular astigmatism is very common and is usually corrected well with glasses or standard contact lenses. Keratoconus causes irregular astigmatism, where the cornea is not simply shaped a bit unevenly, but becomes distorted and unstable over time. This is why people with keratoconus often need specialty contact lenses or corneal treatment rather than routine correction alone.
Keratoconus often begins in the teenage years or early adulthood, but it can also be diagnosed later. Sometimes it is picked up when prescriptions start changing faster than expected, or when corneal mapping is performed for contact lens fitting or laser surgery screening.
Symptoms can start subtly, then become more noticeable as the cornea becomes more irregular. Many patients describe vision that fluctuates and is harder to “lock in” clearly.
Common symptoms include ghosting or double images, shadowing around letters, and distortion that makes straight lines look uneven. Clarity can vary day to day, and some people notice one eye is significantly worse than the other.
Keratoconus can cause rapid prescription shifts, especially in the earlier progressive phase. You might feel like glasses are updated often but still do not give stable crisp vision, or that one eye cannot be corrected as well as it used to.
Glare and halos around lights are common, and night driving can become uncomfortable because car headlights and streetlights may appear smeared or starburst like. These symptoms are often related to irregular astigmatism and higher order optical distortion.
Keratoconus does not have one single cause, but there are known risk factors and associations that can increase likelihood and progression.
Risk is higher if a close relative has keratoconus. Family history does not guarantee you will develop it, but it can be a reason to screen earlier, especially if vision changes quickly or astigmatism increases.
There is a strong association between frequent eye rubbing and keratoconus progression. Allergies that cause itchy eyes can increase rubbing, so managing triggers matters. Conditions like pterygium can also cause surface irritation and redness, so treating ocular surface issues can support comfort and reduce the urge to rub.
Keratoconus is more common in people with atopy, such as eczema, asthma, and hay fever. The link is likely related to inflammation, eye rubbing, and tissue response, rather than being caused by one specific condition.
Keratoconus varies a lot person to person. Some cases remain mild and stable, while others progress and need active treatment. The stage helps guide correction options and monitoring frequency.
In early keratoconus, corneal irregularity may be mild and vision may still correct reasonably well with glasses. Subtle irregular astigmatism can still cause ghosting or night glare even when the prescription looks small.
As keratoconus progresses, corneal shape changes become more obvious and irregular astigmatism increases. Vision can fluctuate, prescriptions may change frequently, and standard correction becomes less reliable. This is often the stage where cross linking is considered to stabilise the cornea.
Advanced keratoconus can cause significant distortion, higher dependence on contact lenses, and an increased risk of corneal scarring. When scarring or severe irregularity limits vision despite specialty lenses, surgical options may be discussed.
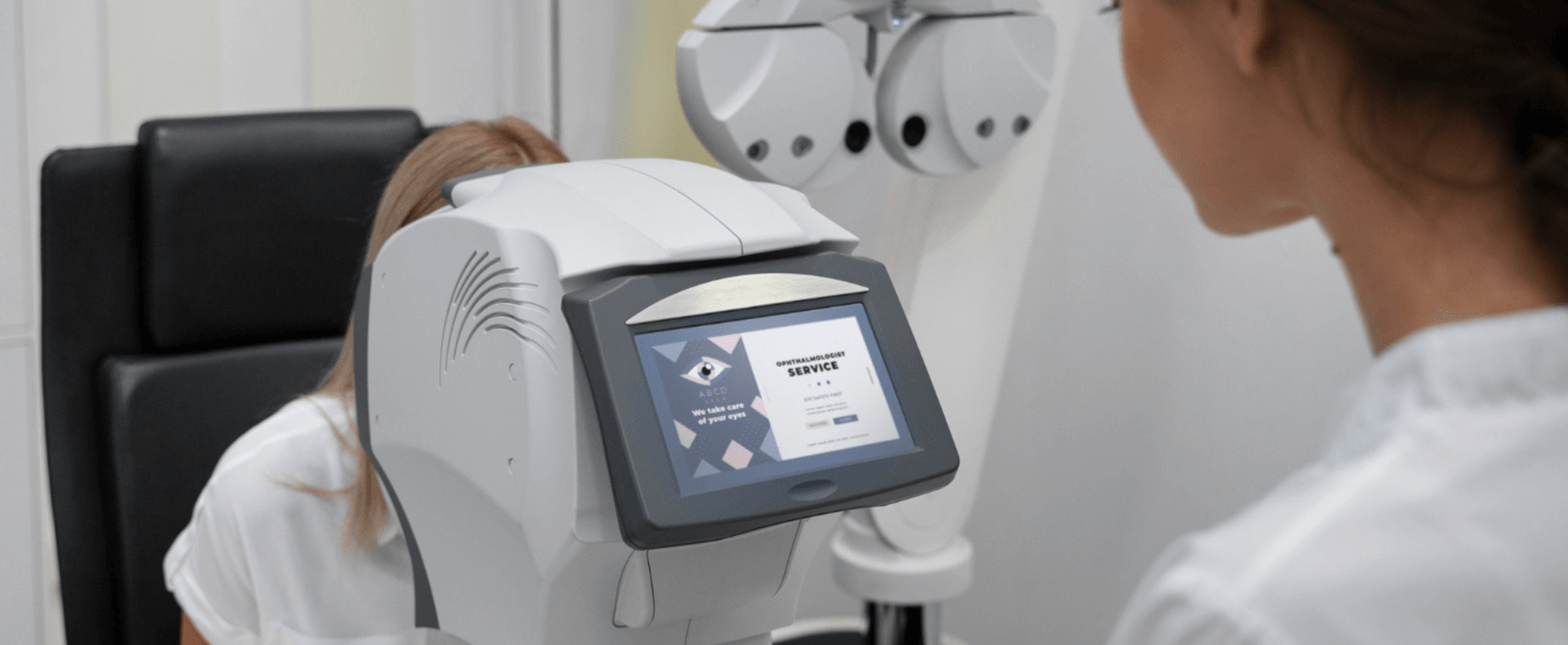
Diagnosis is based on a combination of your symptoms, refraction patterns, and detailed corneal imaging. Corneal mapping is key because keratoconus can exist even when a basic eye test still seems fairly normal.
Topography and tomography map corneal curvature and detect early keratoconus changes. These scans identify steepening, asymmetry, and irregularity that glasses prescriptions alone cannot fully explain.
Pachymetry measures corneal thickness and helps track thinning patterns associated with keratoconus. Thickness data also matters for treatment planning, particularly for cross linking suitability.
Refraction often shows increasing astigmatism, changing axis, or reduced best corrected vision. A key clue is when vision cannot be fully sharpened with standard glasses, or when there is persistent ghosting.
Progression is typically confirmed by comparing scans over time, alongside prescription changes and vision stability. Repeat imaging helps decide when to intervene and how often to review, even if symptoms feel similar.
Treatment depends on stage, progression, and how well vision can be corrected. The focus is usually twofold: stabilise the cornea if it is progressing, and optimise vision with the best correction option for your eyes and lifestyle.
Glasses can help in early keratoconus, especially when irregularity is mild. Even then, some distortion can remain because glasses cannot fully neutralise irregular corneal shape.
Specialty contact lenses often provide the best vision because they create a smoother optical surface over the irregular cornea. Options include rigid gas permeable lenses, hybrid designs, and scleral lenses, which vault over the cornea and can be more comfortable for many people while giving strong visual quality.
Cross linking is designed to strengthen the cornea and slow or stop progression. It does not reverse keratoconus, but it can help preserve your current corneal shape and reduce the chance of needing more invasive surgery later. If you are considering this treatment, our corneal cross linking page explains how it works and what recovery can involve.
In selected cases, corneal ring segments may be used to reshape the cornea and improve lens tolerance or functional vision. This is not suitable for everyone and is usually considered when contact lens wear is difficult but a transplant is not yet the right step.
A corneal transplant may be considered when scarring, severe thinning, or extreme irregularity limits vision despite contact lenses. This is generally reserved for advanced cases and is discussed carefully with expected recovery and long term monitoring. You can learn more about transplant options on our corneal transplant page.
Cross linking is one of the most important treatments to know about because it targets progression rather than just correcting vision.
Cross linking is often recommended when there is evidence of progression, especially in younger patients or when scans and refraction show consistent change. The goal is to intervene early enough to stabilise the cornea before distortion becomes harder to manage.
The main goal of cross linking is stabilisation. Vision does not usually become instantly perfect, and you may still need glasses or contact lenses afterwards. Some people notice gradual visual improvement as the cornea stabilises, but results vary and should be discussed in a realistic way.
Recovery depends on the technique used and your ocular surface. Follow up visits and repeat corneal scans matter because the benefit is measured over time by stability, not by how you feel in the first few days.
Keratoconus management is long term, and the small daily habits can make a real difference to comfort and stability.
If your eyes itch, treating allergies and dryness helps reduce the urge to rub. Cold compresses, allergy management, and avoiding rubbing triggers can be practical steps. If you notice persistent irritation, it is worth discussing it during your review so the ocular surface is not overlooked.
Even if vision feels stable, keratoconus can change gradually. Regular monitoring allows progression to be caught early, and it supports better timing for treatments like cross linking if needed.
Lens optimisation is often the key for daily tasks. Some people need different lens strategies for long screen days versus night driving. Setting realistic expectations is important, especially if glare and halos are part of your baseline symptoms.
Keratoconus care works best when it is both imaging driven and practical for real life vision needs.
Detailed corneal mapping and thickness assessment support earlier diagnosis and better monitoring of progression, which is critical for planning treatment and timing.
Having access to treatments like cross linking and appropriate surgical pathways means care can be matched to stage and risk, rather than relying on correction alone.
To book an appointment, visit your appointment. Bring your current prescription, contact lens details, a brief symptom timeline, and any family history that may be relevant. If you are currently wearing contact lenses, it can help to mention the lens type and how many hours you can comfortably wear them.
Yes. Many people manage keratoconus with glasses in early stages and specialty contact lenses in more advanced stages. Cross linking is a procedure aimed at stabilising progression rather than improving vision correction alone.
Cross linking strengthens the cornea to slow or stop progression in many cases. It is most effective when done early in progressing keratoconus, but outcomes vary and require proper assessment and follow up.
Scleral lenses can provide excellent comfort and visual quality for many people because they vault over the cornea and mask irregular shape. The best lens type depends on your corneal shape, eye surface, and daily tolerance.
Standard laser vision correction is usually not recommended in keratoconus because removing corneal tissue can worsen instability. A suitability assessment is essential, and other options may be discussed depending on your case.
Monitoring frequency depends on age, stage, and whether progression is suspected. People with recent changes often need closer follow up with repeat scans.
A corneal transplant may be considered when vision cannot be improved adequately with contact lenses due to severe irregularity or scarring, or when the cornea becomes too thin or unstable for other options.
Freedom from glasses starts here.

Symptoms can start subtly, then become more noticeable as the cornea becomes more irregular. Many patients describe vision that fluctuates and is harder to “lock in” clearly.
Blurred or distorted vision
Frequent prescription changes
Light sensitivity and night vision problems
Glare and halos around lights are common, and night driving can become uncomfortable because car headlights and streetlights may appear smeared or starburst like. These symptoms are often related to irregular astigmatism and higher order optical distortion.


Keratoconus is more common in people with atopy, such as eczema, asthma, and hay fever. The link is likely related to inflammation, eye rubbing, and tissue response, rather than being caused by one specific condition.
Advanced keratoconus can cause significant distortion, higher dependence on contact lenses, and an increased risk of corneal scarring. When scarring or severe irregularity limits vision despite specialty lenses, surgical options may be discussed.
Corneal tomography
Corneal thickness measurements
Refraction and vision testing
Monitoring for progression
Progression is typically confirmed by comparing scans over time, alongside prescription changes and vision stability. Repeat imaging helps decide when to intervene and how often to review, even if symptoms feel similar.


Glasses (Early keratoconus)
Contact lenses for keratoconus
Specialty contact lenses often provide the best vision because they create a smoother optical surface over the irregular cornea. Options include rigid gas permeable lenses, hybrid designs, and scleral lenses, which vault over the cornea and can be more comfortable for many people while giving strong visual quality.
Corneal cross linking (CXL)
Corneal transplant (Advanced keratoconus)


Managing eye rubbing and allergies
Regular monitoring
Work, screens and night driving
Keratoconus is not a one visit condition. A good plan includes vision correction strategy, monitoring cadence, and clear triggers for when treatment should be considered.
Detailed corneal mapping and thickness assessment support earlier diagnosis and better monitoring of progression, which is critical for planning treatment and timing.
Having access to treatments like cross linking and appropriate surgical pathways means care can be matched to stage and risk.
Rediscover clearer vision
Loacation: G11-12/566 St Kilda Road, Melbourne VIC 3004
Phone: (03) 9070 0955
Fax: (03) 9978 9426
E-mail: info@cityeyesurgeons.com.au
Copyright © 2025 City Eye Surgeons. All rights reserved. Privacy Policy.