Freedom from glasses starts here.
Corneal cross linking is a minimally invasive treatment designed to make the cornea more resistant to ongoing thinning and bulging. It is most commonly recommended when scans and vision measures suggest the condition is progressing over time.
CXL uses riboflavin (vitamin B2) drops and ultraviolet A (UV-A) light. Riboflavin soaks into the cornea and, when activated by UV-A, supports the formation of additional bonds between collagen fibres. This increases corneal stiffness and helps limit further shape change.
CXL is used to manage progressive corneal ectasia, including:
Not everyone with keratoconus needs CXL. The key factor is whether the cornea is changing over time. Common symptoms that can suggest worsening corneal shape include:
Symptoms alone are not enough to confirm progression, but they are a common reason to arrange updated testing and review.
CXL is usually considered when there is documented progression, or when the risk of progression is high and delaying treatment could increase the chance of avoidable vision loss.
CXL is generally most effective when done in early to moderate disease with evidence of progression, before advanced scarring or severe distortion occurs. Younger patients often progress faster, so earlier treatment may be recommended if testing shows change over time.
The best approach depends on corneal thickness, scan findings, lifestyle needs, and specialist preference.
This is the most established method. The surface layer of the cornea (epithelium) is gently removed to allow better riboflavin penetration, then UV-A is applied. A bandage contact lens is typically placed afterwards to improve comfort while the surface heals.
In selected cases, the surface layer is kept intact. This can reduce early discomfort, but riboflavin penetration may be less reliable, so suitability needs careful assessment and discussion.
Accelerated protocols use higher UV-A intensity over a shorter period to reduce treatment time. Your specialist will advise whether this is appropriate for your cornea and clinical situation.
CXL is usually performed as an outpatient procedure. You will be awake, and the eye is numbed with anaesthetic drops.
You can expect pre-operative testing such as:
Contact lens “washout” is important for accurate scans. Exact timing depends on lens type and how your cornea responds, but many clinics use ranges such as days to 1 week for soft lenses and longer periods for rigid lenses. Your surgeon will give you a specific plan based on your lenses and your scans.
For visit planning, you can review what to bring and how to prepare on your appointment page.
While protocols vary, a typical epi-off treatment includes:
Your specialist will also prescribe eye drops for healing and infection prevention.
Time in the clinic is commonly around 1.5 to 2 hours including preparation, riboflavin soaking, and UV treatment time (the UV portion is shorter). Plan for someone to take you home, especially after epi-off treatment, as vision is often blurred and the eye can be light sensitive.
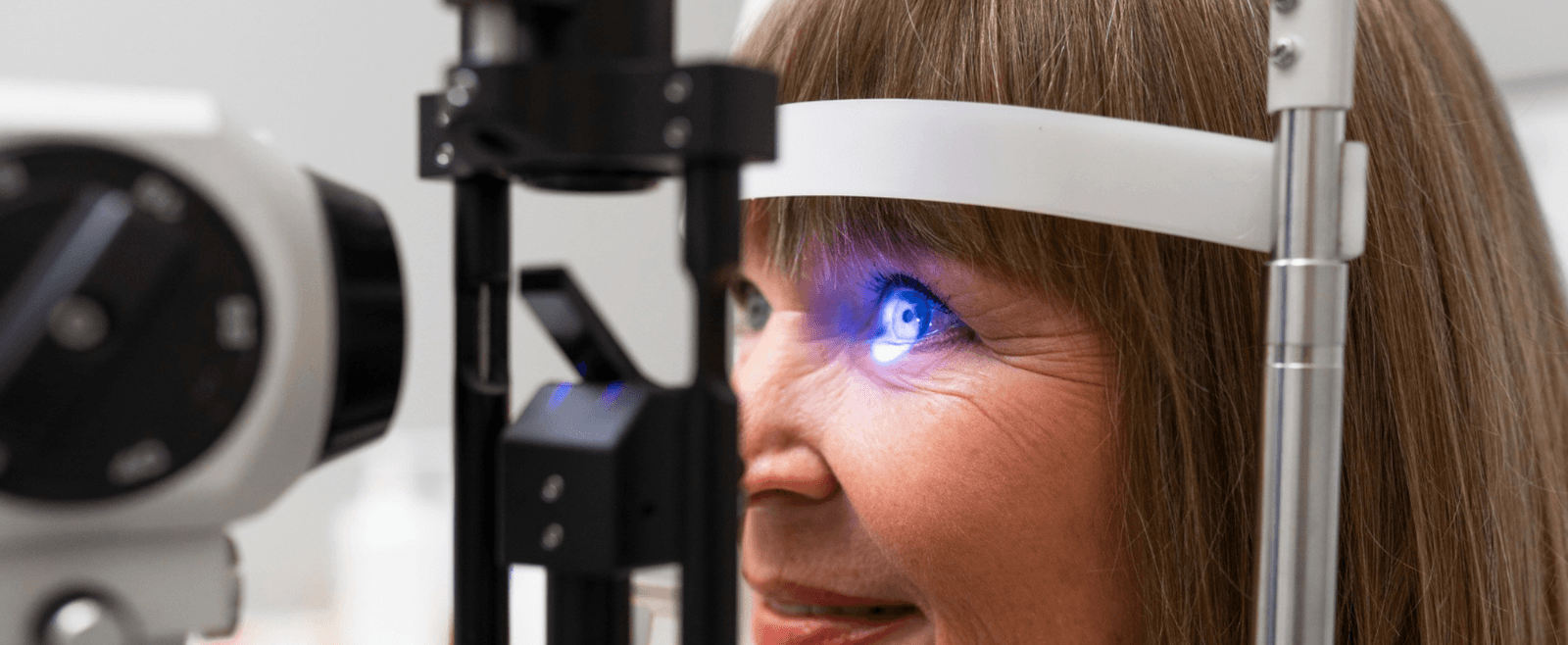
Recovery can feel different between patients, and it also depends on whether epi-off or epi-on was used.
With epi-off CXL, it is common to experience:
Your drop plan often includes an antibiotic, an anti-inflammatory, and lubricating drops. The bandage contact lens is usually removed once the surface has healed, often around the first week, depending on your specialist’s assessment.
Vision often fluctuates early on, then gradually stabilises over months as the cornea remodels. Some people notice clearer vision over time, while others mainly notice improved stability rather than a major vision change.
CXL is primarily done to slow or stop progression. The “success” of treatment is usually measured by corneal stability on follow-up scans and reduced risk of ongoing deterioration.
CXL does not reliably improve vision on its own. Some people see modest improvement in corneal shape or best-corrected vision, but many still need glasses or contact lenses afterwards.
For many patients, the benefits are long-lasting, but ongoing monitoring is still important. Keratoconus can remain stable for years after treatment, and your specialist will advise how often you need scans based on your risk profile.
Glasses and contact lenses improve vision by correcting the way light focuses, but they do not treat progression. CXL targets the underlying biomechanical instability that causes worsening shape change.
Corneal ring segments may be considered in some patients to improve corneal shape and functional vision. They are used for visual rehabilitation and may be combined with CXL in selected cases, depending on the pattern of ectasia and goals of treatment.
A corneal transplant is usually reserved for advanced keratoconus with significant scarring, severe thinning, or contact lens failure where useful vision cannot be achieved otherwise. CXL can reduce the chance of reaching that stage by stabilising the cornea earlier.
We prioritise determining whether monovision is genuinely a good fit for your eyes and your lifestyle. Where appropriate, trial options help you experience it before committing to a longer-term plan.
Monovision works best when expectations are realistic. We’ll talk through what’s likely to feel great, what might feel different, and what matters most for your work, driving, and daily life.
Epi-off CXL often causes moderate to significant discomfort for the first couple of days, with light sensitivity and grittiness during the first week. Epi-on approaches may be more comfortable early, but suitability is case dependent.
Do not drive on the day of treatment. Many people need at least several days to a week before driving, but timing depends on comfort, vision, and healing. Your specialist will confirm when it is safe for you.
Some patients can have both eyes treated, but many clinics prefer to treat one eye at a time so you have a better-functioning eye during early recovery. Your specialist will advise what is safest for your situation.
CXL is intended to stabilise the cornea long term, but it does not “cure” keratoconus. Some patients, especially those with higher risk of progression, may still show changes over time and need ongoing monitoring.
Yes. Many patients continue contact lenses after CXL. Timing depends on healing and lens type. Some guidance suggests scleral lens wear may resume in a few weeks to about a month for existing wearers, but your specialist will give you personalised clearance.
Freedom from glasses starts here.
Corneal cross linking is a minimally invasive treatment designed to make the cornea more resistant to ongoing thinning and bulging. It is most commonly recommended when scans and vision measures suggest the condition is progressing over time.



CXL is usually considered when there is documented progression, or when the risk of progression is high and delaying treatment could increase the chance of avoidable vision loss.
CXL is generally most effective when done in early to moderate disease with evidence of progression, before advanced scarring or severe distortion occurs. Younger patients often progress faster, so earlier treatment may be recommended if testing shows change over time.
At your appointment, you can expect pre-operative testing such as:
Contact lens “washout” is important for accurate scans. Exact timing depends on lens type, and is typically 1 week for soft lenses and longer periods for rigid lenses. You will be given specific advice when booking your appointment.
What to expect during the CXL procedure
Epithelium off cross linking
This is the most established method. The surface layer of the cornea (epithelium) is gently removed to allow better riboflavin penetration, then UV-A is applied. A bandage contact lens is typically placed afterwards to improve comfort while the surface heals.
CXL is usually performed as an outpatient procedure. You will be awake, and the eye is numbed with anaesthetic drops.
Step by step: How corneal cross linking is performed
While protocols vary, a typical epi-off treatment includes:
Your specialist will also prescribe eye drops for healing and infection prevention.
How long does corneal cross linking take
Time in the clinic is commonly around 1.5 to 2 hours including preparation, riboflavin soaking, and UV treatment time. Plan for someone to take you home, as vision is often blurred and the eye can be light sensitive.
The First Week
Vision changes over the first 3 to 12 months
Vision often fluctuates early on, then gradually stabilises over months as the cornea remodels. Some people notice clearer vision over time, while others mainly notice improved stability rather than a major vision change.
Returning to work, driving and exercise


The main outcome: stopping progression
CXL is primarily done to slow or stop progression. The success of treatment is usually measured by corneal stability on follow-up scans and reduced risk of ongoing deterioration.
Will CXL improve vision
CXL does not reliably improve vision on its own. Some people see modest improvement in corneal shape or best-corrected vision, but many still need glasses or contact lenses afterwards.
How long does cross linking last
For many patients, the benefits are long-lasting, but ongoing monitoring is still important. Keratoconus can remain stable for years after treatment, and your specialist will advise how often you need scans based on your risk profile.
A corneal transplant is usually reserved for advanced keratoconus with significant scarring, severe thinning, or contact lens failure where useful vision cannot be achieved otherwise. CXL can reduce the chance of reaching that stage by stabilising the cornea earlier.
Glasses and contact lenses improve vision by correcting the way light focuses, but they do not treat progression. CXL targets the underlying biomechanical instability that causes worsening shape change
Epi-off CXL often causes moderate to significant discomfort for the first couple of days, with light sensitivity and grittiness during the first week.
Do not drive on the day of treatment. Many people need at least several days to a week before driving, but timing depends on comfort, vision, and healing. Your specialist will confirm when it is safe for you.
Many clinics prefer to treat one eye at a time so you have a better functioning eye during early recovery. Your specialist will advise what is safest for your situation.
CXL is intended to stabilise the cornea long term, but it does not “cure” keratoconus. Some patients, especially those with higher risk of progression, may still show changes over time and need ongoing monitoring.
Yes. Many patients continue contact lenses after CXL. Timing depends on healing and lens type.
If you have keratoconus or suspected corneal ectasia, a consultation can confirm whether your condition is stable or progressing and whether CXL is appropriate.
To book, please contact us. If you have prior scans, bring them along, and if you wear contact lenses, bring the details of your lens type and current prescription.
Rediscover clearer vision
Loacation: G11-12/566 St Kilda Road, Melbourne VIC 3004
Phone: (03) 9070 0955
Fax: (03) 9978 9426
E-mail: info@cityeyesurgeons.com.au
Copyright © 2025 City Eye Surgeons. All rights reserved. Privacy Policy.